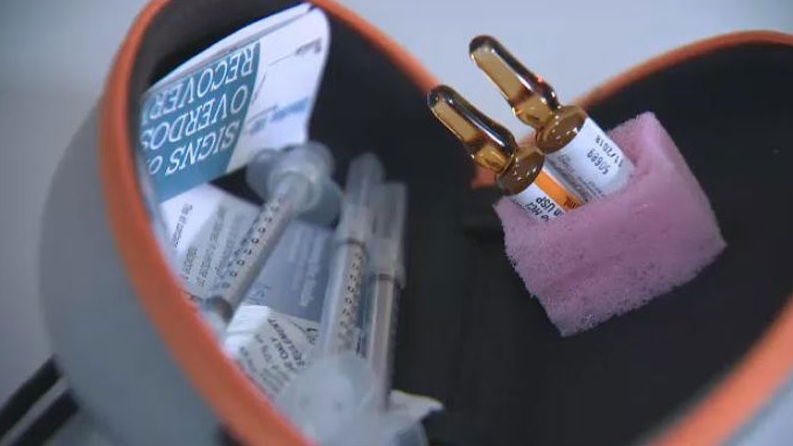
HALIFAX -- Nova Scotia is taking initial steps to head off a British Columbia-style epidemic of fentanyl overdose deaths.
The province's chief medical officer of health said $1.1 million will be spent to distribute about 5,000 free kits with naloxone -- an antidote for opioid overdoses -- through police, jails, and community pharmacies.
"It's critical we have these in place as we're faced with increasing amounts of fentanyl and other synthetic opioids on our streets," said Dr. Robert Strang Friday.
He said making the naloxone available is part of "the first important steps in a long journey" that is likely to see yet more fentanyl flood into the drug distribution networks of the East Coast province.
About 60 people died last year from opioid overdoses in Nova Scotia, including four who were killed by illicit fentanyl.
Since several pilot projects with naloxone were started last year, health officials estimate the drug has saved about 30 people from dying from opioid drug overdoses.
Strang said $564,000 of the total spending will extend the availability of naloxone into community pharmacies and harm reduction clinics in Sydney, Truro and Halifax.
Three community-based organizations that distribute needles and information to addicts will receive the remaining money. A total of $160,000 will go to Northern Health Connections in Truro; $247,000 for Mainline Needle Exchange in Halifax; and $152,000 to Sharp Advice Needle Exchange in Sydney.
"I'm up in the clouds. This news was so welcome," said Diane Bailey, executive director of Mainline Needle Exchange, who attended the announcement.
Bailey said some clients are telling her they're using fentanyl, while others that they've seen it around the streets.
She said her agency's site will be able to extend the reach and hours of its mobile clinics, as well as the amount of time it spends in rural areas.
"Our next step is to train our outreach staff to be trainers, to provide overdose prevention, education ... so we can distribute naloxone to people who use our service," she said.
Fentanyl has the potential to kill a wide cross section of users, including those who consume it accidentally when it is mixed in with other opioids such as crack cocaine.
"This is not just about people who are established opioid drug users. It could be even a young person in school who is a first time drug user," said Strang.
The public health physician said the funding is an "immediate response," while a wider plan that a task force is working on should be ready in a few weeks.
Strang also said an assessment is currently being carried out to consider whether to set up a supervised, safe-injection site in the province.
"So when you talk about a safe consumption site ... we're in the process of working through that, and we haven't made an application (to the federal government)," he said.
Another area under consideration by the task force Strang is co-chairing is how to reduce the practice of many doctors of prescribing high levels of prescription opioids for pain relief.
Figures provided to The Canadian Press indicate that last year 2,246 Nova Scotians received big-dose prescriptions of highly addictive painkillers, though about one fifth of those were cancer patients who may need larger dosages for end-of-life care.
These are dosages of opioids equivalent to about 200 milligrams or more per day of morphine -- enough to cause a fatal overdose to a newcomer to the drug.
Dr. Gus Grant, the registrar of the province's College of Physicians and Surgeons, has said the figures indicate a large cohort of patients are being maintained on dosages of medicine that aren't supported by medical evidence and exposes them to health risks exceeding the benefits.
The Nova Scotia college has adopted as "best practice" a guideline from the U.S.-based Centers for Disease Control and Prevention to avoid doses in excess of 90 milligrams.
Every six months, physicians with the highest risk profiles are contacted and given a detailed description of their prescribing habits. They are also given resources to assist them in considering their prescribing practices.
However, the college hasn't decided to set firm standards for doctors prescribing the opioids, as now exist in British Columbia.
A spokesperson from the college was unavailable for comment Friday, while Strang said the matter is being considered, without a definite date for action.
"It's more complex than setting a hard, rigid rule. We need to walk through it carefully," said Strang.